Workforce Management, PCAS, and The RFP Process
Greater adoption of health information technology (HIT) provides opportunities to use electronic staffing and patient classification/acuity systems (PCAS) to go beyond inflexible ratios. It also gives visibility to factors influencing staffing needs, such as varying levels of patient care requirements, nurse skill mix and patient assignments. Here are three key concepts to consider when evaluating clinical case management software solutions.
Workforce Management | PCAS | RFP Process | Annotated References & Acknowledgments | PDF Version
Workforce Management
Principles, Values, Responsibilities
Staffing impacts the ability of all nurses to deliver safe, quality care at every practice level and in all practice settings:
- Nursing care delivery is multifaceted
- Appropriate nurse staffing determination is complex1,2
Nurses have a professional duty to be knowledgeable about staffing, its processes and organizational functions, as part of their responsibility to patients. While nurse managers and other leaders may be accountable to their organization for nurse staffing, all nurses are accountable to their patients and profession.3
Nurse leaders seek to make appropriate staffing assignments by matching resources to patients based on3:
- patient care needs
- staff skill mix
- education
- competencies
- unit variables
- Much of the process can be automated1
Today, everyone from the CNO to the frontline nurse must understand the relationship between staffing, cost, and patient, staff and organizational outcomes.
There are four phases to the staffing process:
- Forecasting
- Scheduling
- Staffing
- Improving
Scheduling and staffing operationalize the budget plan, while the process of improving and adjusting based on this analysis ensures the delivery of safe quality care in a cost effective manner.
Staffing and scheduling systems ease every phase of the process:
- Systems translate policies, staffing data and evidence into business rules to drive schedule creation
- Automated systems assist in promoting staff satisfaction surrounding perceptions of fairness for the actual work schedule along with the process used to generate that schedule4
- Systems facilitate effective communication, active staff participation and increase staff autonomy and satisfaction
- Systems alert managers of variances and urgent staffing issues, and provide dashboards and reports that help monitor productivity
- Systems simplify and automate the processes that increase efficiency and provide reliable and valid data to decision-makers across many units/departments and settings
Forecasting
Shape a plan for current and future operational requirements by analyzing organizational structure and policies, operational variables, and staffing data.
|
Element |
Description |
Software Considerations |
Implications |
|
Core component of the workforce management process at an organizational level. |
Components, generic process, examples, considerations, dependencies. |
When evaluating workforce management to support this phase, check for: |
Contributor < - - - - - > Process Driver |
|
Establish workforce vision |
Establish evidence-based shared vision for staffing & desired outcomes. At the core of any workforce management forecasting/budgeting/planning process should be a patient-centric vision including the care delivery model and an understanding of standardized versus unit-level staffing policies |
Alignment of vendor philosophy to organization goals of workforce management |
|
|
Project staffing needs |
Collaborate with financial team to project census/volume predictions for fiscal year that includes growth and decreases by service line and strategic initiatives and allocate them to the unit/department level |
Integration with financial planning software |
|
|
Set staffing levels |
Identify minimum and maximum staffing levels and required staffing by unit/department using desired HPPD and acuity benchmarks |
Fields and process to record min and max levels and integrate HPPD and acuity benchmarking |
|
|
Determine skill mix |
Calculate coverage needs by skill and credentials based on care delivery model |
Integration to human capital system |
|
|
Check for adequate coverage |
Ensure adequate flex for on-boarding/turnover, sick/vacation coverage – adjust upward for overtime and/or agency traveler use. Creating a reasonable budget number that takes all factors into account is crucial to success |
Algorithms to support calculation |
|
Scheduling
Determine a set number and type of staff to be allocated for an anticipated workload and defined future time period, typically four to twelve weeks. Translate budget and forecast into a tactical plan for meeting expected patient volumes, service and care requirements.
|
Element |
Description |
Software Considerations |
Implications |
|
Core component of the workforce management process at an organizational level. |
Components, generic process, examples, considerations, dependencies. |
When evaluating workforce management to support this phase, check for: |
Contributor < - - - - - > Process Driver |
|
Establish scheduling policies |
Set policies based on evidence-based shared vision for staffing & desired outcomes. Consider: fairness, responsibility for scheduling, timeframes, regulatory/union requirements |
Flexibility in scheduling rules |
|
|
Plan for coverage of non-productive hours |
Account for non-productive hours in the scheduling process and determine how you will meet demand: overtime, float pool, agency, etc. |
Support inclusion of staff not primarily assigned to a unit, into that units scheduling process |
|
|
Build schedule |
Determine core staffing model and build schedule, shifts and staffing grid based on forecast with flexibility to match updated volumes and patient needs |
Intuitive user interface |
|
|
Review scheduling rules |
Review scheduling rules particular to specific schedule period. Competency based schedules require balancing of skills and core coverage during high and volume metrics |
Robust rules engine to translate policies into scheduling rules
|
|
|
Schedule staff |
Assign staff to open shifts based on needs and staff preferences, or open schedule for staff self-scheduling |
Scheduling interface that matches methodologies used within the organization |
|
Staffing
Day-to-day operations that assess and determine the shift allocation of nursing resources to ensure adequate staffing on each shift and unit/department. Typically occurs within 4 to 48 hours of the work shift.
|
Element |
Description |
Software Considerations |
Implications |
|
Core component of the workforce management process at an organizational level. |
Components, generic process, examples, considerations, dependencies. |
When evaluating workforce management to support this phase, check for: |
Contributor < - - - - - > Process Driver |
|
Establish staffing policies |
Set policies based on evidence-based shared vision for staffing & desired outcomes. Consider the need to facilitate and maintain coverage when unexpected events occur (i.e., weather, unplanned absences, low volume, high volume, sitter needs, and no shows). Be sure to include the need for RN oversight of staffing, particularly at the shift and unit/department level |
Flexibility in staffing rules |
|
|
Assess patient needs |
Assess patient needs for upcoming staffing period. Patient needs may be measured as acuity, intensity, or workload. Projected needs should be updated via RN assessment of patient needs (acuity) and transformed into a staffing requirement. Ongoing changes and anticipated patient flow and demand variability should be incorporated |
Inclusion of patient need (acuity) in staffing modeling |
|
|
Match staffing to patient needs |
Fairly and equitably match staff to patient needs across the organization. Minimize or eliminate open shifts. Match staff competencies and skills appropriately. Fill open shifts. Communicate staffing changes throughout organization |
Organizational level view of enterprise staffing needs |
|
|
Coordinate support staff |
Staff supplemental resources (such as agency and sitters) |
Support staffing components Communication with external contract labor systems |
|
|
Assign nurse to patients |
Assign nurses to care for particular patients based on complexity of care needs and continuity of care |
Nurse-patient assignment capabilities |
|
Improving
Monitor, analyze and evaluate staffing actions to plan in real-time, near-time and retrospective intervals. Identify trends and patterns that inform and refine scheduling and forecast planning.
|
Element |
Description |
Software Considerations |
Implications |
|
Core component of the workforce management process at an organizational level. |
Components, generic process, examples, considerations, dependencies. |
When evaluating workforce management to support this phase, check for: |
Contributor < - - - - - > Process Driver |
|
Track data |
Record information needed to determine compliance to policy, desired outcomes to assess evidence-based shared vision for staffing. (Assess compliance T&A, etc.) |
Reporting and analytics capabilities |
|
|
Monitor now |
Review time-stamps to track current staffing levels to patient needs in real time |
Analytics to support: |
|
|
Incorporate into scheduling |
Align schedule effectiveness to optimize shift and scheduling process |
Analytics to support: |
|
|
Feed strategic planning |
Analyze long-term workforce trends and correlations to staff satisfaction and patient outcomes. Loop findings into resource allocations and deployment as part of strategic planning |
Analytics to support: |
|
Patient Acuity/Classification Systems (PCAS)
Determining the right number and type of nursing staff required to meet patient care needs historically is viewed as the foundation of workforce management systems5,6. From Florence Nightingale's initial efforts to assign patients to particular wards based on severity of illness7 to more focused studies from the 1960's forward, the need for accurate data on patient care requirements has continued to grow.
- Data impact all aspects of workforce management:
- Forecasting
- Scheduling
- Staffing
- Improving
- Directly affects patient care quality, safety, and effectiveness by compensating for shift variations in care needs
- "A growing body of evidence shows that patient acuity-driven staffing is an effective way to optimize nurse staffing to improve patient outcomes and promote clinical and organizational excellence"8.
Terminology
The term Patient Classification Systems refers to measurement systems in nursing that reflect actual patient care needs for staffing purposes. The term also is referred to as Acuity Systems, although the concept of "Acuity" denotes unidimensional illness severity in the medical sense. A literature review demonstrates that the majority of the nursing community continues to prefer the more inclusive term Patient Classification to reflect the broader bio-psycho-social-spiritual mandate of nursing. Therefore, for purposes of this discussion, the term Patient Classification/Acuity System is used.
Operational Definition
A Patient Classification/Acuity System (PCAS) is defined here as "the methods and processes of determining, validating and monitoring individual patient care requirements over time in order to assist in such determinations as: unit staffing, patient assignments, case mix analysis, budget planning and defense, per patient cost of nursing services, variable billing and the maintenance of quality assurance standards"9:
- Includes critical system elements as well as various ways the resulting data can be used.
- confirms that a tool or measure with rules and definitions is used to determine patient care requirements
- includes processes for validating and monitoring the measure and its outcomes over time
- PCAS data uses:
- unit staffing
- equal workload distribution
- quality of care maintenance
- budget development
- costing out care
- organizational processes
Types of Patient Classification/Acuity System Measures
Three basic types of PCAS tools can be identified, with different philosophical assumptions. Each type defines nursing care for the organization and aims to capture the fluctuations in patient care requirements in a different way. Each tool type is designed to connect to staffing and scheduling in a various ways, with the goal of assuring the right number and type of staff needed to care for any given patient group.
Prototype Tools
The first type of PCAS measure is the Prototype approach. This method describes different patient care levels in general terms such as "Minimum, Moderate, or Maximum care" and is often accompanied by care levels, such as "1= Minimum Care, 2= Moderate Care, and 3= Maximum Care." A brief description of the different care requirements at each level is usually provided as well. The determination of the patient care level is ultimately a subjective matching of the actual care needs with the prototype description that most closely matches the actual patient care requirements. As such, there is no actual tool that gets completed9,10. This approach has also been defined as "a descriptive method using several mutually exclusive and exhaustive categories of care"11.
Staffing by patient ratios or grids can also be viewed as another Prototype approach. However, as Bolton and her colleagues pointed out,12fixed staffing numbers or ratios only identify minimum staffing levels and do not adjust for the ever changing nature of patient care needs. As such, ratios alone are insufficient for staffing purposes.Summative Task Tools
The second major type of PCAS measure is known as the Summative Task approach>. These measures are task and frequency-based and assume that patient care requirements are best expressed as the sum of a series of observable tasks and activities. Each task is assigned a weight or number of points that is ultimately expressed as an increment of time such as minutes or hours. Those minutes or hours are added up, converted to hours, and are used to project the number of staff that generally equate to those hours9,10.
Care Interaction Tools
The third type of Patient Classification/Acuity measures are known as Care Interaction tools. This approach to PCAS is based on conceptually distinct categories of patient care requirements or attributes rather than on individual tasks or activities. The critical indicators associated with this type of measure assume that patient care requirements are a function of a complex interaction between various objective and subjective critical predictors of care such as the "type, frequency, duration, and complexity of the particular patient care requirements". Care Interaction tools view patient care as greater than the simple sum of individual patient care tasks and as such require the greatest degree of professional judgement of the PCAS tool types9,10.
Design Principles for Patient Classification/Acuity Systems
Important Design Principles have been identified for PCAS13. These Design Principles include the following:
Validity and Reliability
Validity and reliability are perhaps the most important yet misunderstood elements of the Design Principles. A Patient Classification/Acuity tool or measure is considered valid if it actually measures what it is designed to measure, and in this case that means different levels or amounts of patient care that vary in the predicted direction.For example, assume that a nursing unit is using a level 3 PCAS tool, with level 1 representing minimum care, level 2 indicating a moderate level of care, and a level 3 representing the maximum amount of care on a unit. If patient care is then studied and the results show that on average, patient care increases with each increase in patient care level, that result is direct evidence of validity. So if a study shows that level 1 patients get less care than other level patients, and a level 2 patient gets more than a level 1 but less care overall than level 3 patients, the tool is valid because that the care varies in the predicted directions. Using a Patient Classification/Acuity tool that does not have established validity is to be avoided at all costs because of the lack of credible evidence that the tool actually works, even when staff are using it correctly. Using invalid PCAS measures will result in erroneous and incomplete estimates of actual patient care requirements, potentially affecting projected staffing levels and the resulting care quality. Validity should always be well established using sound research methods when a tool is first developed and periodically thereafter. The moral and scientific responsibility to create valid tools falls to the developing organization, whether an individual hospital, healthcare system, or private company offering the PCAS on the open market.
Reliability of a Patient Classification/Acuity tool means that if the measure is valid and being used correctly, the results of the ratings should be accurate and dependable. For example, if three different nurses who all know the care requirements of a particular patient separately rated his care needs using the same valid Patient Classification/Acuity tool, they should all choose the same indicators and end up with the same patient rating. When a tool is dependable and you can count on the ratings being correct, it is considered to be reliable.
It is also extremely important to understand the critical relationship between validity and reliability. A tool might start out with strong evidence of validity, but if it is used incorrectly, the ratings will become incorrect and thus unreliable. Unreliable ratings automatically render any PCAS tool invalid. This crucial relationship must be well understood from the start and form the basis for ongoing staff education and reliability and validity monitoring for PCAS tools and measures over time.The importance of validity and reliability for PCAS tools cannot be overstated. In fact, it has been observed that Patient Classification/Acuity System measures have all too often lacked evidence of validity and reliability9,10,14,15. In order to assure that the PCAS tools used in healthcare are as sound as possible, the validity and reliability of these systems should be well established when it is initially developed and/or purchased, and the ongoing reliability of patient ratings should be assessed at least annually for every staff member rating patients with a given measure. In addition, a description of the research methods used to demonstrate validity and reliability should be provided and reviewed before implementation in a healthcare setting is seriously contemplated.
Simplicity and Efficiency
The need for simplicity and efficiency in a Patient Classification/Acuity System is critical to maintain overall system effectiveness and not add unnecessarily to nursing's workload. To that end is the scientific principle of parsimony, capturing the totality of care with as few indicators as possible, thereby achieving the gold standard of simplicity and elegance. Practically speaking, this means that more items or indicators on a tool are not necessarily better13. In fact, the Simplicity and Efficiency Design Principle can only be met by a PCAS tool "that is conceptually clear, concise, and time-efficient to use" 9,10 . Simplicity, efficiency, and the visibility of the tool and its indicators ultimately drive the overall usefulness of the measure.PCAS measures that are embedded in the documentation systems of an electronic health record (EHR) are often in the background and not immediately visible to the nurse. As with any type of PCAS under consideration, it is critical that the nursing members of the system selection team see a total listing of the tool indicators, the associated weighting scheme, as well as a full description of the methodology so that they understand exactly how the care levels are calculated. Patient Classification/Acuity Systems should never be selected without this type of demonstration and level of understanding. This process will also assist in determining how much the system meets the Simplicity and Efficiency Design Principle.
Objectivity
Another important Design Principle to look for in a Patient Classification/Acuity System is that it should allow for ease in objective verification of tool ratings as well as the tool validation process13. This can be best achieved by having someone with both nursing and measurement expertise involved in the development of the measure.Acceptability
It has been observed that the acceptability of PCAS measures is important to colleagues both inside and outside the nursing department. For members of the nursing team, acceptability is a function of how well the measure appears to capture the essence of nursing and patient care. This also implies the exercise of subjective nursing judgement in rating patient care needs13. When the Patient Classification/Acuity System is acceptable to nursing, acceptability in other critical departments such as Finance will occur as they are also educated about the system, how it can be used, the selection process and rationale, as well as ongoing system monitoring processes9,10. The importance of this step is crucial to any healthcare organization because of the important assertion that "valid and reliable PCAS's define and defend the work of professional nursing practice, protect patients from complications, and decrease the vulnerability of nurse staffing to budget cuts"17. As such, the care indicators on a PCAS tool must be visible and represent the full scope of nursing practice and patient care.Tool Development
It is essential that when a Patient Classification/Acuity System is under development that a registered nurse with doctoral level expertise in measurement methods or an RN working directly with someone with that expertise has been involved throughout the tool development process. This helps assure that patient care and nursing's scope of practice are well understood and represented by the Patient Classification/Acuity measure. It also assures stronger validity and reliability of the PCAS tool at the start. In addition, access to registered nurse clinical experts for feedback and testing throughout the development process is also critical if the system is to appropriately define nursing care and meet the intent of this critical Design Principle.Nursing Work
This final Design Principle offered by Fasoli, Fincke, and Haddock13 is fundamental to a well-conceived, fully relevant Patient Classification/Acuity System for nursing. This principle involves the common knowledge and central belief that nursing work is much greater than the simple sum of individual tasks. Keeping this core knowledge and understanding of the interactive nature of nursing practice in mind and making sure it is incorporated throughout the system development, application, and utilization phase will help assure a system that works for nursing, the organization, and the patients it serves.
Keys to Successful Implementation
In order to fully implement and maintain a Patient Classification/Acuity System so that it informs staffing decisions in the most complete way, eight Keys to Successful Implementation reflecting best practices in evidence-based leadership must be applied to the process9,10,18,19. The eight keys are:
Commitment
Create and foster high level commitment to make the system work as well as it possibly can at all levels of the organization. Starting with the nursing leadership team, enthusiasm can be encouraged by education about the system and how it can help each nurse, patient, and the organization on a daily basis. Commitment is contagious. Since commitment is evidenced by action, assessing commitment levels of all staff should be an ongoing process so that it can be influenced as needed.Clarity
Assure there is widespread clarity and understanding about the purpose of the Patient Classification/Acuity System. Some staff might worry that the new system could result in layoffs or decreased staffing. One of the major messages that staff can't hear often enough is that purpose of the new system is to assure appropriate staffing, given the actual patient care needs. Also reminding managers and staff that a valid and reliable Patient Classification/Acuity System is one of the best ways to document the staffing that is actually required. That particular point should encourage staff to rate patients as carefully and correctly as possible so that care requirements will be visible to all.Coordination
Appoint one person with an appropriate level of authority to serve as the organization's Patient Classification/Acuity System Coordinator, with responsibility for the implementation and ongoing oversight and maintenance of the system over time. Department and shift level staff coordinators should be designated and also work closely with the organization PCAS Coordinator so that annual reliability and validity assessment can be scheduled and conducted as part of ongoing competency validation. By meeting on a regular basis, any problems that surface can be identified and resolved in a timely manner.Education
Education is a major key to successful implementation and long term maintenance of any Patient Classification/Acuity System. All levels of staff need to have a common knowledge base about the system, its purpose, and their role in making it work. This core information needs to be offered in a variety of ways over time to meet learner needs. The PCAS and staffing requirements should be routine agenda items for general staff meetings. Issues can be resolved much easier when they are made known sooner rather than later. It is also essential that PCAS training be a core component of the On-boarding process. Organizations might even consider acknowledging individual staff or units with high PCAS reliability scores on a periodic basis.Expertise
Build staff and coordinator expertise in using the PCAS must be a major organizational goal. Devising ways to transfer that expertise to other levels of staff will help assure organizational strength and redundancy in this critical skill set. Instituting an Expert User program where strong staff expertise related to the PCAS is assured in all departments and shifts is one important way organizations can invest in their staff in a new and important way.Involvement
All levels of nursing management and staff must be involved in the implementation and long-term maintenance of the Patient Classification/Acuity System. This involvement may look differently across staff levels, but it is critical to implementation success. It has been said that "the earlier and more widespread the involvement, the more successful the implementation" 9,10. This approach also fosters immediate problem identification and remediation.Communication
Multiple venues for communication about the system in an ongoing way is the best way to assure successful implementation of the PCAS. Whether the issue is related to staffing, the nursing budget, or patient care issues, there are likely implications for the Patient Classification/Acuity System that can be addressed, whether in shift report, staff meetings, issues forums, or in impromptu staff discussions. Engaging in regular, direct communication about the PCAS is one of the best ways to insure successful implementation over the long term.Evaluation
In addition to annual reliability monitoring of the staff involved in rating patients and periodic formal validity assessments of the PCAS, accurate patient ratings should be an expectation spelled out in every appropriate staff and manager level job descriptions and performance evaluations. This approach helps assure that the PCAS knowledge base of staff and managers is current and correct, contributing to optimal system performance and application over time.
Integration of Patient Classification/Acuity Systems
The goal of integration should be simple: minimizing time and maximizing benefits. This relies on being able to access and repurpose data in one system to drive data results in another, without redundancy and errors. It is this outcome that creates system integration and drives efficiencies and effort. Currently, there are three major sources of Patient Classification/Acuity Systems:
- A healthcare organization can develop its own PCAS that is unique to that organization. If the organization already has a Staffing and Scheduling System, patient ratings from the newly created PCAS may be integrated with the additional functions of the existing staffing system.
- A healthcare organization can also choose to acquire and implement a vendor neutral PCAS that works with any EHR and Staffing and Scheduling System.
- A healthcare organization may choose the PCAS that comes with the Staffing Scheduling System and/or EHR they currently use or are purchasing.
Regardless of the source of the PCAS, the Design Principles and Keys to Successful Implementation outlined in this work should be fully utilized to make this critical decision. It is also important to note that each of the three sources of a PCAS involves some work to integrate the system both within and across an organization.
The decision to integrate disparate systems in information technology may be a complex process, depending on the characteristics of the systems involved. Determining what data elements are needed as well as the timing and automation of such outcomes, is critical to the overall success. System integration links together different computing models and software applications, whether physically or functionally, to act as a coordinated whole.
Within Healthcare, there are many sustainable, stand-alone systems that produce the intended results, and bridging the gap between systems successfully creates an integrated platform where the sum is greater than that of each individual solutions. It is important to keep in mind that all data from two systems does not need to be integrated in order for the desired results to be achieved. The key driver is the overlapping data points that need to be identified, and where these data elements can be found across the organization's software continuum. Bringing together diverse data and sources from smaller components into a single solution allows the resulting software to continue functioning as one system.
Integration and Interface are terms that are often used interchangeably, but are two different strategies. Interface languages and middleware allows systems to communicate regularly, with specific timeframes and data points. Integration is more far-reaching, basing its complexity on "near or real-time" transfer of actual data, component granularity, data integrity and over-arching organizational goals.
Staff shortages, continuing cost inflation and service demand have intensified the call for more effective and efficient use of scarce resources through integrated service delivery models20,21. A "systems-integration approach that incorporates the fundamental building blocks of healthcare, from equipment and technology to clinical insight and workflow processes, is needed to take the next major leap in improving quality and safety."22
Additional Considerations
One of the unanticipated outcomes of implementing a PCAS is the collaboration it requires with other service areas and disciplines and the resultant opportunities provided. The ability to create data and workflows that are easily transposed to multiple service areas and cross-functional teams underscore the process and ultimate outcomes of the organization. When designing a Patient Classification/Acuity System tool, common threads across the organization's multiple applications exist that allow for synergies to form. These touch points need to "connect the dots" between the patient, diagnosis, care plan changes, the patient stay experience, and any outpatient or discharge planning . The flow and understanding that aligns with the patient registering at the hospital to their discharge all has downstream ramifications in the care continuum.
The goal of determining these common threads across applications is to ultimately provide a Patient Classification/Acuity measurement based on patient demand that can accommodate staffing needs as well as guide other decisions such as bed placement and discharge planning . All levels of nursing have a stake in this process:
- At the Executive Level, issues related to patient safety, financial stability of the organization, and the need for systems that support improved patient throughput and placement are critical.
- For Nursing Management, financial implications of patient throughput, bed availability, staffing and length of stay are crucial concerns, as are aligning staffing to patient care needs, workload, and regulatory compliance. Managing overtime and Agency usage are also important areas of focus.
- For Staff Nurses, common threads related to equal workload distribution, staff qualifications, overtime, and patient safety will also be areas of interest.
By allowing clinical teams to explore the workflow of cross-functional solutions together, common threads that are present as well as any deficiencies can be identified and evaluated so that staff resources and patient care requirements can be better aligned. Focusing on these themes will allow for improved workflow, staffing effectiveness, as well as alignment of the nursing work team overall. Once system improvements are made, the promise of Patient Classification/Acuity Systems can begin to be realized.
The Request for Proposal (RFP) Process
Prior to writing an RFP, assess current organizational systems and processes to identify requirements of a new system that will be procured.
Understanding the organization's needs will help:
- identify the appropriate vendor candidates, and
- allow vendors to better demonstrate appropriate software solutions.
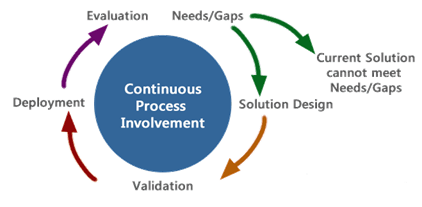
The RFP Process
Steering Committee Selection
Select a Committee leader who believes in the project, has the time to participate, and who can effectively communicate and facilitate communication.
Sample members of the team could include:
- IT leadership representative
- Nursing leadership
- Human Resources
- Finance
- Operations
- Ancillaries
Clarify Goals / When to RFP
Clarify Goals:
- The team will need their collective expertise to define what current systems cannot do today and if a new system is being considered.
- Reaching out to similar health care organizations and understanding what their solutions are may be helpful.
When to RFP
- Evaluate current assets/systems in relationship to needs.
- Research vendors offering solutions which align with organizational goals.
Benchmarks
Set program benchmarks that can be tracked in order to accurately measure program success.
Benchmarks allow vendors to have a clear understanding of what is desired from the system.
Benchmarks may include:
- Clinical/Quality Benchmarks (typically for acuity and patient classification tools)
- Patient satisfaction with pain management
- Patient satisfaction with nursing care
- Patient satisfaction with overall care
- Patient satisfaction with medical information provided
- Pressure ulcers
- Patient falls
- Nurse job satisfaction
- Rates of nosocomial infections
- Total hours of nursing care per patient, per day
- Staffing mix (ratios of RNs, LPNs, and unlicensed staff)
- Staffing Benchmarks (typically for staff scheduling tools)
- Core/Contingency utilization
- FTE commitments
- Extra/Overtime
- Core staff floating
- Shift cancelations
- Contingent Labor Benchmarks (typically for vendor management solutions)
- Staff quality
- Fill rates
- Time to fill
- Cancellation Rates
- Vendor Performance
Need/Gap Analysis
Definition: a documented list of pain points and new requirements for the system being pursued, with the appropriate documentation from the benchmarks and from the steering committee.
- Technical gaps are data and/or application functionality that does not exist today or is fundamentally flawed (ie, the staffing office does not have the ability to see all open shifts across inpatient nursing areas).
- Process gaps are missing or broken operational workflows in the hospital related to the target system (ie, vacation requests are submitted by nurses on paper forms that are easily lost).
Guiding Principles: Help clarify the reason and drivers for the decision-making process during the RFP vendor selection. Guiding principles generally fall into one of four categories
| CATEGORY | SAMPLES |
|---|---|
| Operational Drivers |
|
| Technical Drivers |
|
| Patient Care Drivers |
|
| Other Factors |
|
RFP Components
Steps to define your purpose
- Use the work from the Steering Committee and create a clear list of defined goals that the selected vendor should meet.
- Clearly define what problem needs to be solved and what solutions are being sought. Do you need a core scheduling application? Do you need to also manage contingent labor including temps and contractors?
Expect your RFP to contain
- Functionality/filling outcomes
- Cost: acquisition and maintenance
- Technical Requirements
- Infrastructure
- Support
- Legal
- Compliance
- Accreditation
- Regulatory
Avoiding Common Pitfalls
Skipping the RFI process
- Narrowing down the list of vendors to roughly 5 during the RFP process is critical.
- A simple Request for Information (RFI) can help you weed out the bad fits.
- RFI's are the process of requesting general information from software vendors about their products and solutions they provide, without the rigor of lengthy requirements scoring and demonstrations.
- Some vendors use an approach (like integrated timecards and schedules) or a technology (like cloud or mobile) that easily qualifies or disqualifies them from your search.
- Ask questions that force participating companies to provide answers that speak to your stated objectives.
Internal confusion and conflict.
- When internal committee members and decision makers agree early on goals for the RFP, it avoids conflict.
- Not everyone gets what they want, but decisions made that align with the overall goals of the project will guide one solution over another.
Asking unnecessary questions.
- Make sure every question on the RFP has a clear purpose.
- This will make for sharper responses from vendors and sharper judgements from your team.
- Ask open ended questions like "How would the system perform xyz process?" instead of "Can you do xyz function?"
- Yes/No questions are not valuable for differentiating vendors from each nor for understanding how their strengths fit your guiding principles.
- Open ended questions let you understand how the vendor approaches the solution, but from a usability and an overall strategic perspective.
Unrealistic timelines.
- Be realistic how long the RFP should take and don't try and rush the process.
- On larger RFPs, vendors should have at least 4 weeks to form a response to an RFP in order to ensure the highest level of quality in the response.
Poor benchmarking
- Does the criteria align with the stated goals of the project? If it doesn't, the information necessary to assess the solution against the decision making factors won't be gained.
Ignoring key stakeholders
- Make sure the committee consists of multiple stakeholders that represent all areas of the health system that will be affected by the change.
- Managing change is easier when stakeholders feel invested in the process.
Vendor Selection
- IT leadership representative
- Nursing leadership
- Human Resources
- Finance
- Operations
- Ancillaries
Steering Committee
Create scoring criteria and schedule demonstrations that will facilitate a final vendor selection.
Scoring:
- Create an evaluation team and assign roles. Consider creating teams of subject matter experts to review each section with a final review team to make final evaluations and resolve any disputed scores.
- Ensure that evaluators are not allowed to communicate with vendors during the evaluation period.
- Have a clearly defined scoring system that is transparent to vendors and creates an opportunity to standardize the quality of vendors when compared against one another.
- Standardize scoring. A scale of "1 to 3" or "1 to 5" works well:
- 5 points = Fully meet requirement
- 4 points = Meets requirement, but has minor issues
- 3 points = Meets requirement but has more significant issues that may require moderate level of compromise
- 2 points = Partially meets requirement and has significant issues that may be hard to overcome
- 1 point = Does not meet requirement
- Prioritize scoring. Two questions that receive a 5 are not necessarily created equal. Each question can have a level of priority assigned. The higher the priority, the less likely a compromise is accepted. Break the RFP up into sections that you can assign value to. Each section could be assigned a percentage of value. For example, if there are 4 sections, one may be worth 50% of the overall score, while the other 3 combined make up the other 50%.
- Decide how much of a role price plays into the score. Don't let it become a main factor.
- Plan sufficient time for scoring the RFP.
- Identify top vendors for Demos
Demonstration
The best processes are basic and include a list of all functionality grouped into sections, such as:
- Scheduling
- Communication
- Interfaces
- Licensure
- Open Shift Management
- Staffing
- Reporting
- End-User Experience
- Training
Questions relative to these sections should be provided in advance of the demo and used as a guide for the demo ahead of time.
- Demo sessions should be interactive
- Have a moderator in place to keep track of time and ensure that all areas are covered in the allotted time – typically two to three hours.
Deployment and Evaluation
Creating system requirements: After researching staffing solutions, identify which companies publish offerings that align with your requirements. Your team should be able to speak to staffing required to implement and maintain your solution, technical infrastructure, maintenance, and support, in addition to core functionality.
Annotated References & Acknowledgments
Annotated References
-
Avalere Health LLC. (2015 September). Optimal nurse staffing to improve quality of care and patient outcomes. American Nurses Association White Paper. Retrieved from: www.nursingworld.org/Avalere-WhitePaper-on-NurseStaffing
-
Mensik J. (2014, February). What every nurse should know about staffing. American Nurse Today, 9(2). Retrieved from: www.americannursetoday.com/what-every-nurse-should-know-about-staffing
-
American Nurses Association. (2012). ANA's Principles for Nurse Staffing, 2nd ed. Silver Spring, MD: American Nurses Association.
-
Wagner, K., Lee, F. W., & Glaser, J. P. (2013). Health Care Information Systems A Practical Approach for Health Care Management. San Francisco: Jossey-Bass.
-
Behner, K., Fogg, L., Frankenbach, J., & Robertson, S. (1990). Nursing resource management: Analyzing the relationship between cost and quality in staffing decisions. Health Care Management Review, 15(4), 63-71.
-
Mark, B., Burleson, D., (1995). Measurement of patient care outcomes: Data availability and consistency across hospitals. Journal of Nursing Administration, 25(4), 52-59.
-
Abdellah, F., Levine, E. (1979). Better patient care through nursing research. 2nd Ed., New York, NY: McMillan.
-
O'Keefe, M. (2016). Practical steps for applying acuity-based staffing. American Nurse Today, 11(9), 30-34.
-
De Groot, HA. (1989). Patient classification system evaluation: Essential system elements: part 1. Journal of Nursing Administration, 19(6), 30-35.
-
De Groot, HA. (1989). Patient classification system evaluation: System selection and implementation: part 2. Journal of Nursing Administration, 19(7), 24-30.
-
Malloch, K. (2013). Patient classification systems: State of the science 2013. Nurse Leader, 11(6), 35-37.
-
Bolton, L, Jones, D., Aydin, C., Donaldson, N., Brown, D., Lowe, M., McFarland, P., Harms, D., (2001). A response to California's mandated nursing ratios. Journal of Nursing Scholarship, 33(2), 179-184.
-
Fasoli, D., Fincke, M., Haddock, K. (2011). Going beyond patient classification systems to create an evidence-based staffing methodology. Journal of Nursing Administration, 41(10), 434-439.
-
Adeylotte, M. Nurse staffing methodology: A review and critique of selected literature (No NIH 73-433). Superintendent of Documents, U.S. Government Printing Office.
-
Fasoli, D., Haddock, K. (2010). Results of an integrative review of patient classification systems. Annual Review of Nursing Research, 28, 295-316.
-
Giovanetti, P. (1978) Patient classification systems in nursing: A description and analysis. Springfield VA: National Technical Information Service; 1978.
-
Malloch, K. (2012). Changing tides: Evidence to embrace a patient classification system. Nursing Economics, 30(6), 356-358.
-
De Groot, HA (1994). Patient classification systems and staffing: part 2, Practice and process. Journal of Nursing Administration, 24(10), 17-23.
-
De Groot, HA (2005) Evidence-based leadership: Nursing's new mandate. Nurse Leader, April, 37-41.
-
Fleury, M.J. (2006). "Integrated Service Networks: The Quebec Case." Health Services Management Research 19: 153-65.
-
Powell Davies, G.P. (1996). Chapter 1: Integration: An overview. In G. Powell Davies, L. Betbeder-Matibet, A. Nicholls, F. Reynolds, M.A. Bonney, V. Traynor and G. Lucas, eds., General Practice Integration: A Literature Review. Centre for General Practice Integration Studies, University of New South Wales.
-
Matthews, S. and Pronovost, P. (2011). The need for systems integration in health care. Journal of the American Medical Association, 305 (9), 934-35).
Additional Resources
Carnegie Mellon University (n.d.). Software system integration. Retrieved from: www.sei.cmu.edu/productlines/frame_report/softwareSI.htm
Techwell (n.d.). Effective methods for software and systems integration. Retrieved from: www.cmcrossroads.com/article/effective-methods-software-and-systems-integration
Acknowledgments
This endeavor was sponsored by the American Nurses Association. ANA wishes to acknowledge the following individuals for their expertise in the development of this product:
- John Alis, Senior Consulting Sales Executive (Cerner)
- Scott Allison, Manager, Marketing & Communications, Consultant (Avantas)
- Deborah Crist-Grundman, BSN, RN, Senior Clinical Strategist (Catalyst Systems)
- Holly De Groot, PhD, RN, FAAN, Chief Executive Officer (Catalyst Systems)
- David Faller, Vice President Nursing Solutions (QuadraMed)
- Chris Flanders, Director Healthcare (Axsium)
- Amy Garcia, MSN, RN, Director and Chief Nursing Officer (Cerner)
- Nick Haselwander, Marketing Director (ShiftWise)
- Karlene Kerfoot, PhD, RN, NEA-BC, FAAN, Chief Nursing Officer (API Healthcare a GE Company)
- Bre Loughlin, BN, RN, Clinician (Epic)
- Beth Meyers, RN, PhD(c), CNOR, Chief Nurse Executive & Analytics Strategy Director (Infor Healthcare)
- Danielle Miller, PhD(c), MSN, RNC-OB, C-EFM, Chief Nursing Officer (Infor Healthcare)
- Gia Milo-Slagle, Director, Product Management: Capacity and Workforce Solutions (McKesson)
- Shane Parker, RN, Co-Founder (ShiftWizard)
- Jacob Robinson, Software Developer (Epic)
- Pam Sapienza, RN BSN, MBA, FACHE, Director of Healthcare (Navigant)
- Gaylyn Timiney, MSN, RN, Senior Clinical Operations Consultant (Kronos)
- Heather Wood, Senior Product Manager (QuadraMed)
ANA Staff
- Mary Jo Assi, DNP, RN, NEA-BC, FNP-BC, FAAN
- Nick Blencowe
- Elizabeth Franzino
- Sharon Morgan, MSN, RN, NP-C